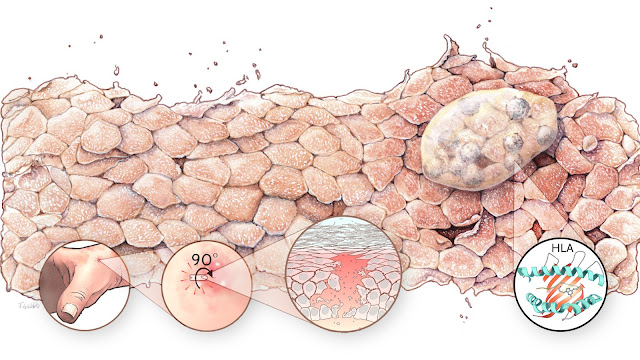
USU Researcher Creates Lab and Biorepository to Study Dermatology’s Most Deadly Diseases
By Vivian Mason
“Many people tend to think of dermatology as mainly acne problems, basic skin ailments, and beauty issues,” says Dr. Helena Pasieka, assistant professor of Dermatology at the Uniformed Services University’s (USU) F. Edward Hébert School of Medicine. However, this often misunderstood specialty is much more than that. Skin is the human body’s largest organ, and some skin diseases can be deadly.
Among them is Stevens-Johnson syndrome (SJS) and the more severe Toxic Epidermal Necrolysis (TEN), two forms of the same life-threatening disease that are triggered by severe adverse skin reactions to a variety of medications. SJS and TEN cause a rash similar to a second-degree burn, as well as sores on the mucous membranes and eyes.
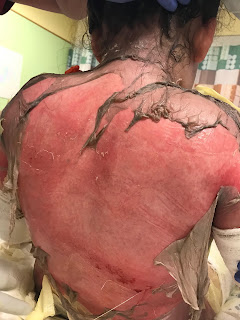 |
| Patient exhibiting acute stage of SJS/TEN. (Photo credit: Dr. Helena Pasieka, USU) |
As both an internist and dermatologist, Pasieka practices complex medical dermatology, where the patients are more ill or medically complicated. Before coming to USU, she worked with these patients at MedStar’s Georgetown University Hospital, Washington Hospital Center, and the National Rehabilitation Hospital in Washington, D.C.
Individuals affected by SJS and TEN are typically hospitalized in a burn unit or an intensive care unit. Skin peeling is the hallmark of these two conditions, wherein the top layer of skin sometimes peels off in sheets from large areas of the body. SJS and TEN are on a spectrum of severity, with SJS causing small areas of peeling skin (affecting less than 10% of the body) and TEN causing large areas of peeling skin (affecting more than 30% of the body); SJS/TEN overlap is in the middle of the severity spectrum. The affected areas are very painful, and the patients become very ill.
“I partnered with the Burn Center at Washington Hospital Center to help me take care of these patients,” says Pasieka. “TEN is an allergy that occurs when you take a medication, and the body triggers autoimmunity that causes rejection of your skin. Then, the skin sloughs off like a burn.” Pasieka said it is one of the most deadly dermatological diseases and its mortality rate is greater than 30%.
Pasieka wanted to find out more about why these conditions occurred and what was going on biologically. Her intent was to identify two things: a treatment that could be utilized quickly to minimize the amount of skin that falls off and to understand why it’s happening and be able to predict and prevent it entirely.
Within the last year, Pasieka has started setting up a translational science lab at USU. Her main goal is to create a biorepository to collect SJS and TEN patient tissue and data about their hospitalizations, biosigns, blood work, and lab tests. She hopes to receive patient samples from across the country.
“I plan to use total body photography, which we use a lot in dermatology for melanoma,” Pasieka explains. “It provides head-to-toe photos that look at spots and at cancer. I plan to repurpose the total body photography machines to get really good photographic images, almost like obtaining a CAT scan of the outside of a person’s body. I’ll be able to use all the resources at USU to better understand the pharmacology and genetics of SJS/TEN.”
It’s still in its infancy, but Pasieka hopes to hire a postdoctoral scientist and a clinical research coordinator―her dream team. The postdoctoral scientist would help create the biorepository and assist with developing the scientific inquiry that she wants to implement, while the clinical research coordinator could direct writing, maintain protocols, ensure all the proper institutional review board (IRB) protections to safely take information from patients, and manage recruiting patients for study participation.
“I want to make sure we’re doing a safe job of protecting their contributions to science,” Pasieka adds. She also offers education on early diagnosis of the condition, and optimal treatment and healing of the wounds.
Once the kinks are ironed out, Pasieka hopes to open up the biorepository to institutions across the country and even around the world. Many people have already expressed interest in what the lab could offer. “It would be wonderful to get as many samples as possible,” she remarks.
“I’ve already partnered with some of the institutions within the military. It all translates to good military readiness and care of the warfighter. I think being able to respond to the most critical need in anyone’s specialty is a part of that mission, too.”
Pasieka is optimistic that the lab will start receiving samples within the next six months.
“Then,” she says, “we get to do the fun part, which is to ask good questions and use science to figure out what’s going on with these patients. Ideally, we want to know how to protect them, how to help them heal, and how to prevent the condition in the first place.”
And while the biorepository is a major part of Pasieka’s work, she keeps a busy schedule, seeing patients, assisting the attendings and residents with rounds, and teaching residents at Walter Reed, often giving commentary on more complicated medical dermatology cases. She also sees patients in the USU Family Health Center and currently provides certification for the Advanced Trauma Life Support (ATLS) course, all as part of a larger attempt to reframe the narrative on dermatology.
“It’s important for me to lean into the mission here at USU,” Pasieka says, “and also to broaden people’s perceptions of what a dermatologist is and what we can do. It’s not merely taking care of skin in an outpatient setting; we can also take care of people in the ICU and patients in the field.”
As a dermatologist who never did a dermatology rotation in medical school and who initially wanted to be a surgeon, Pasieka appreciates so many things about where she is now.
“I'm thrilled to have the opportunity to combine my dual training in both internal medicine and dermatology into complex medical dermatology and hospital-based dermatology,” Pasieka says. “I feel like I’m always becoming a better doctor and a stronger team member.”
“I’m thankful for the opportunities to take care of the sickest patients in dermatology, to identify their needs, and to know how to best impact their care. It’s important to ask really useful and pertinent scientific questions about how to prevent, treat, and heal SJS/TEN. USU has provided me with the resources and support to take my work to the next level, and I am so thrilled to be here.”
*Banner image: We acknowledge Dr. Elizabeth Phillips from Vanderbilt University Medical Center and Thao P. Do from the PGRN Hub for the use of this image.